🔑 Key Learning
- Viral exanthems present with characteristic rashes and systemic symptoms; quarantine advice varies depending on the condition
- Chickenpox and shingles are caused by VZV; shingles affects a single dermatome and doesn't cross the midline
- Measles and rubella are highly contagious and require exclusion periods after rash onset
- Erythema infectiosum (slapped cheek) is not infectious once rash appears, but poses risks to pregnant women
- Scarlet fever presents with classic features including strawberry tongue and sandpaper rash; treat with penicillin
- Bacterial and parasitic infections such as impetigo, scabies, and head lice have specific treatments and variable exclusion advice
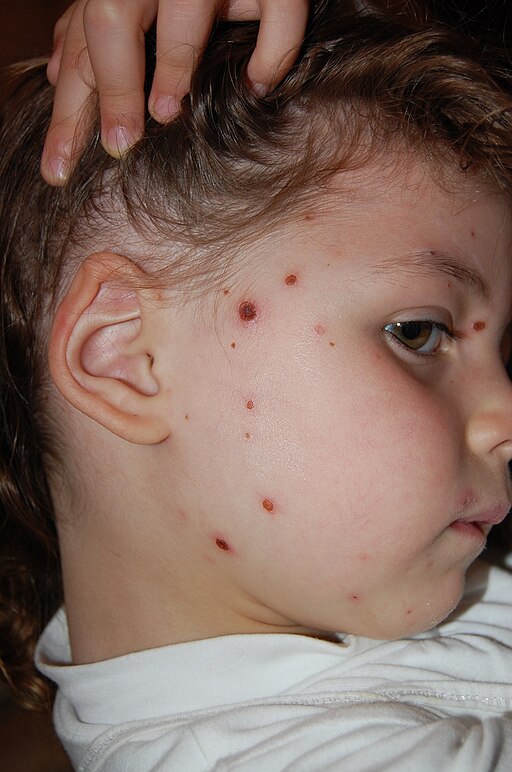
🐔 Chickenpox (Varicella Zoster Virus)
- ✨ Itchy macules → papules → vesicles → crusting in crops
- Rash begins on face/trunk and spreads to limbs
- Exclusion: Until all vesicles have crusted (approx. 5 days after rash)
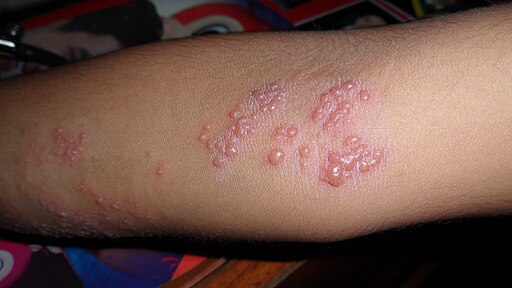
🔥 Shingles (Herpes Zoster)
- Reactivation of VZV in dorsal root ganglia
- Prodrome: Dermatomal 'burning' pain
- Rash: Dermatomal vesicles, unilateral, doesn't cross midline
- Management:
- Oral antivirals (aciclovir) within 72h if age >50, non-truncal, immunocompromised, or severe pain
- Pain control: Paracetamol + NSAID/codeine → if ineffective, consider amitriptyline/gabapentin if needed
.
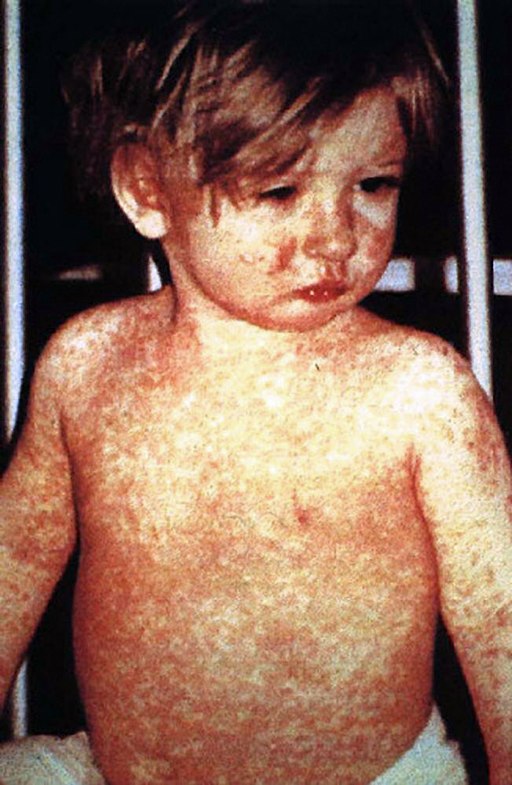
🍚 Measles (RNA Paramyxovirus)
- Prodrome: Irritable, conjunctivitis, Koplik spots (grain of salt appearance on buccal mucosa)
- Rash: Morbilliform, starts behind ears → trunk - maculopapular 'blotchy' rash.
- Exclusion: 4 days after rash onset
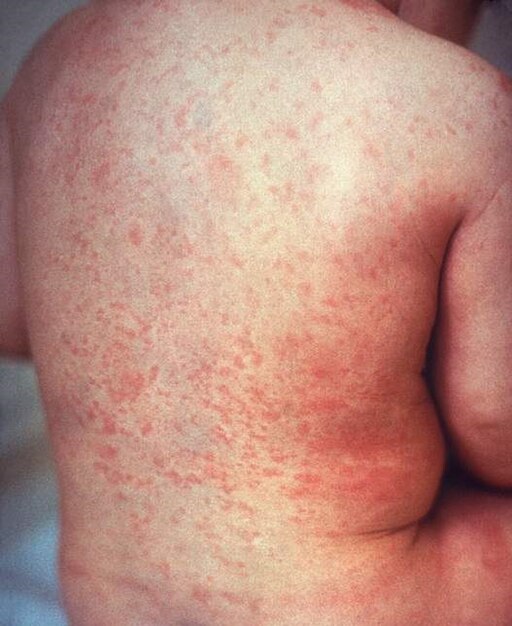
🏛️ Rubella (Togavirus)
- Pink maculopapular rash from face → trunk, resolves rapidly by day 3-5
- Suboccipital/postauricular lymphadenopathy
- Exclusion: 6 days after rash appears
🌹 Erythema Infectiosum (Parvovirus B19)
- "Slapped cheek" rash, spreads to arms/body
- Rash may reappear when warm (e.g. bath time), lasts weeks
- Pregnancy risks: foetal anaemia, hydrops fetalis
- Exposed pregnant women should be informed to see their GP/midwife. Check bloods:
- Recent or current infection is indicated by IgM positive - refer to specialist for close foetal monitoring, growth scans to observe for the above complications.
- IgG and IgM both negative - not immune and therefore susceptible to infection
- IgG positive & IgM negative - immune - reassure of immunity
- Exposed pregnant women should be informed to see their GP/midwife. Check bloods:
- Exclusion: Not required once rash appears
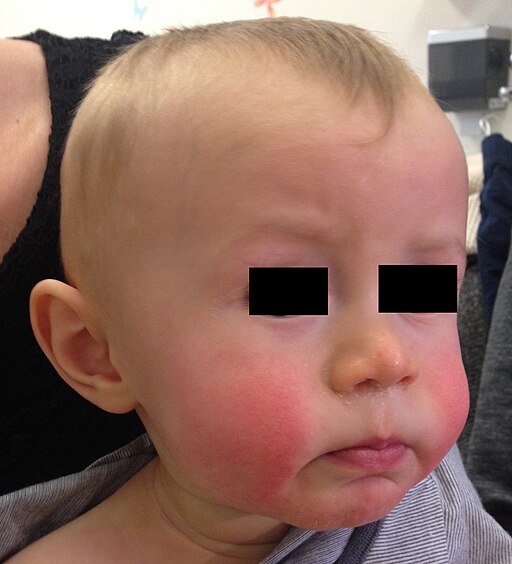
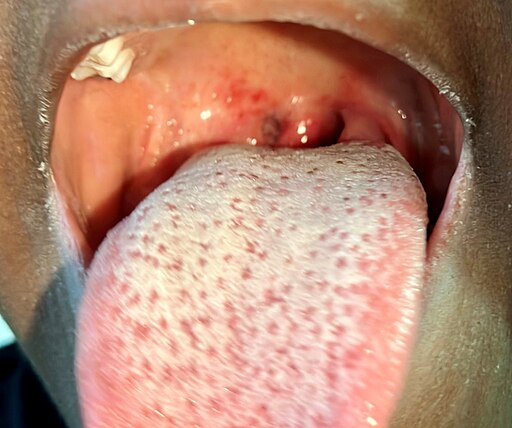
🍓 Scarlet Fever (Strep pyogenes)
- 4 S's: Sore throat, Strawberry tongue, Sandpaper rash, 'S'ircumoral pallor
- Pastia’s lines - accentuated redness in the flexor creases - axilla, inguinal folds, elbows etc.
- Management: Phenoxymethylpenicillin (Pen V) for 10 days
- Exclusion: 24h after starting antibiotics
.
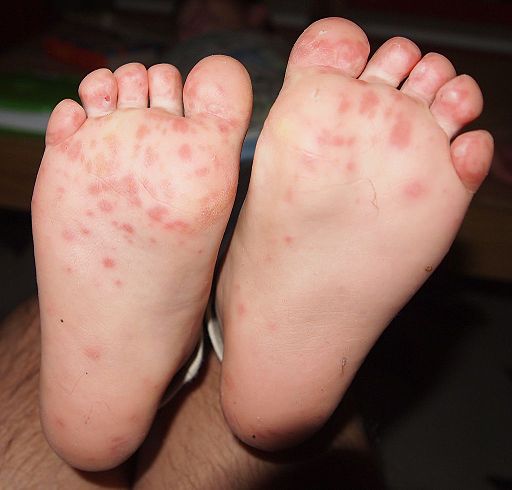
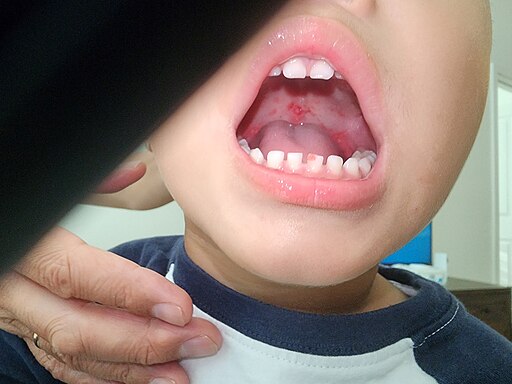
✋👣 Hand, Foot & Mouth Disease (Coxsackie A16)
- Sore throat, fever
- Red blisters on palms/soles; painful mouth ulcers
- Management: Supportive
- Exclusion: Not necessary
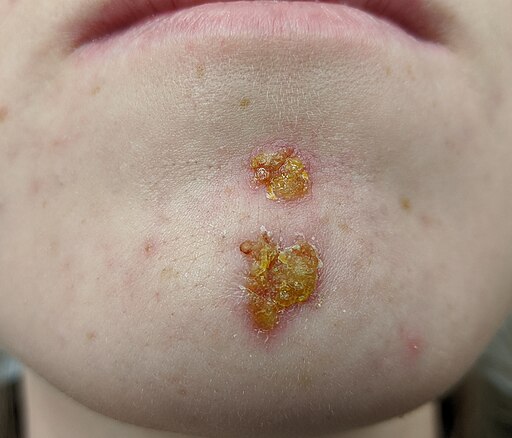
🧈 Impetigo (S. aureus / S. pyogenes)
- Most commonly on the face, around the mouth or on the extremities
- Macule develops into pustule/vesicle which then ruptures. The fluid dries forming a golden, honey-coloured crust, referred to as ‘cornflake lesions'
- Lesions are itchy, sometimes painful
- Impetigo can be bullous with blisters/vesicles
- Management:
- Non-bullous: 1st line - Hydrogen peroxide
- Alternative: fusidic acid/mupirocin
- Extensive disease: PO flucloxacillin
- Bullous impetigo or extensive disease / systemically unwell: Oral flucloxacillin
- Exclusion: 48h or until crusted
- Non-bullous: 1st line - Hydrogen peroxide
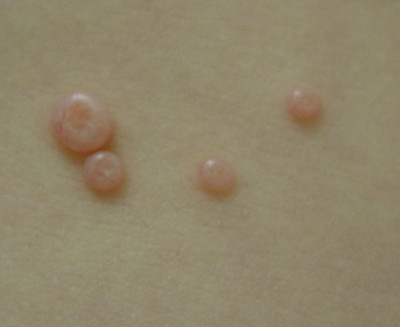
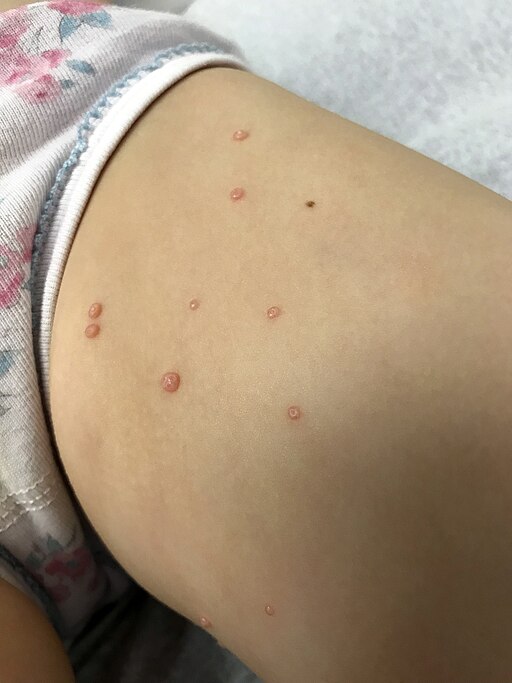
🫧 Molluscum Contagiosum
- Dome-shaped, pearly papules with central umbilication
- Often in clusters, trunk/flexures
- Management: Conservative; resolves in 12-18 months
- Exclusion: Not required
.
🐛 Scabies (Sarcoptes scabiei)
- Intense nocturnal itch, family/close contacts affected
- Disturbs sleep
- Crowded conditions - nursing home, prison etc.
- On examination
- Erythematous papules most commonly distributed in the interdigital spaces, periumbilical area, hands, wrists, axilla, buttocks etc.
- Thin, grey lines 0.5-1.0cm may be seen - the mites burrows
- Management: 1st line - Permethrin 5% once weekly x2 doses, treat all contacts
- 2nd line: Malathion
- Exclusion: Until first treatment completed

🐜 Head Lice (Pediculus humanus capitis)
- Itchy scalp
- Detection: Combing for live lice
- Management: Wet combing, dimeticone 4%, malathion
- Exclusion: None required

📝 Exam Clues & Clinchers
- Chickenpox: Itchy crops of vesicles with crusting at different stages
- Shingles: Painful, dermatomal rash not crossing midline
- Measles: Koplik spots, sore throat, conjunctivitis, blotchy rash
- Scarlet Fever: Sandpaper rash + strawberry tongue, sore throat, sircumoral pallor
- Slapped cheek: Parvovirus B19 + pregnancy alert
- Impetigo: Golden honey crusts - topical hydrogen peroxide if mild, PO flucloxacillin if extensive
- Molluscum: Umbilicated, pearly papules
- Scabies: Burrows in interdigital spaces + itch at night. 1st line: Permethrin 5%
📆 Memory aid - exclusion criteria
- MMR - Measles, Mumps, Rubella = 4, 5, 6
- Measles - 4 days after rash
- Mumps - 5 days after swelling
- Rubella - 6 days after rash
