🔑 Key Learning
- Red flags: not sitting by 8 months, not walking by 18 months, or early hand preference (<1 year)
- Common causes: cerebral palsy (UMN), spinal muscular atrophy (LMN), Duchenne muscular dystrophy (myopathy)
🚩 Early Years Red Flags
- Floppy, poor head control
- Unable to sit unsupported by 8 months
- Asymmetry of motor skills - e.g. hand preference before 1 year
- Not walking by 18 months
- 💡 Tip: 8, 1, 18
🧬 Causes
- Central motor deficit – cerebral palsy, SMA
- Myopathy – Duchenne muscular dystrophy
- Spinal cord lesions – spina bifida
- Global delay – syndromes, unidentified causes
🧠 Cerebral Palsy
A chronic disorder of movement and/or posture that typically presents at < 2yrs. May be accompanied by disrupted development of cognition, communication etc.
Pathology
- Static injury to developing brain → movement/posture disorder
- Causes:
- 80% antenatal – cerebrovascular haemorrhage, congenital infection
- 10% - hypoxic-ischaemic injury (birth asphyxiation)
- 10% post-natal – meningitis/ encephalitis/ head trauma. Hypoglycaemia
Clinical Features
- Abnormal limb/trunk posture + tone
- Abnormal gait
- Unable to sit without support by 8 months
- Asymmetric hand function/preference before 12 months
- Suggests hemiplegia
- Feeding difficulties – due to oromotor incoordination, gagging
Subtypes
- Spastic: increased tone, brisk reflexes
- Dyskinetic: dystonia, choreoathetosis
- Ataxic: cerebellar features
🧬 Spinal Muscular Atrophy (SMA)
Pathology
- AR mutation in SMN1 → anterior horn cell degeneration → LMN syndrome
Clinical Features
- Floppy baby
- Tongue fasciculations
- Symmetric weakness, hypotonia
- Hyporeflexia, bulbar signs
💪 Duchenne Muscular Dystrophy (DMD)
The commonest type of muscular dystrophy - 1/3000 males.
Pathology
- X-linked recessive
- Molecular abnormality of dystrophin → progressive myofibre degeneration
Clinical Features
- Commonly presents around 4-5yrs age – waddling lordotic gait
- Abnormal gait - flat footed, persistent toe-walking
- Delayed motor milestones and speech problems
- Calf pseudohypertrophy – replacement of muscle fibres by fat and fibrous tissue
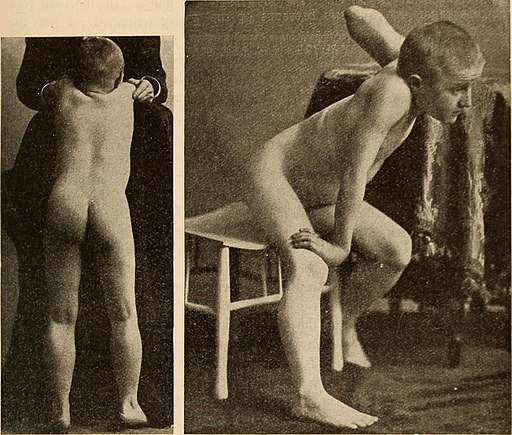
- Weakness in limb girdles (lower esp.) – Gower’s sign
- Uses hands and arms to ‘walk up’ their own body from a squatting position due to lack of hip and thigh muscle strength.
- Progressive atrophy - no longer ambulant by 10-15yrs
Investigations
- Raised CK
- Genetic analysis
💪 Becker Muscular Dystrophy (BMD)
Pathology
- X-linked recessive
- Same allele affected as DMD, but some functional dystrophin production is maintained - as a result, patients have milder features with later onset and slower progression.
Clinical Features
- Diagnosed later than DMD ∼11 yrs
- Mild early symptoms – fatigue, exercise cramps
- Proximal weakness → shoulder girdle later
- Patients are typically ambulatory until late twenties, and LE until mid-old age.
Complications
- Dilated cardiomyopathy
📝 Exam Clues & Clinchers
- Spastic CP: early hand preference, scissoring, UMN signs
- SMA: floppy baby, tongue fasciculations, absent reflexes
- DMD: Gower’s sign, calf hypertrophy, delayed milestones
- BMD: similar to DMD, but slower progression and later onset
